How serotonin mediates psilocybin’s effects for mental health
TL;DR:
- Psilocybin primarily binds to serotonin receptors like 5-HT2A, inducing neuroplasticity rather than increasing serotonin levels. Its effects depend on receptor-specific pathways that restructure neural circuits, explaining its therapeutic potential beyond traditional antidepressants. Individual responses and long-term benefits are shaped by complex receptor interactions, brain circuits, and subjective experiences, making research and safe use approaches crucial.
Most people assume that psilocybin works the same way antidepressants do: by flooding the brain with more serotonin. That assumption is not just incomplete, it actively obscures what makes psilocybin one of the most scientifically interesting substances in modern mental health research. Psilocybin does not raise serotonin levels. It mimics serotonin at specific receptor sites, triggering cascades of brain activity that reshape neural circuits in ways that conventional treatments rarely achieve. Understanding the receptor-level mechanics behind this process is what separates informed, intentional use from guesswork, especially for Canadians exploring psilocybin for mental health enhancement or personal growth.
Table of Contents
- What serotonin really does: Beyond ‘more equals better’
- Psilocybin’s action: Receptor-specific effects and neural pathways
- Debates and breakthroughs: Is 5-HT2A enough to explain everything?
- Implications for mental health, personal growth, and safety
- Why most guides miss the real point about serotonin and psilocybin
- Learn and explore psilocybin’s benefits safely in Canada
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Receptor-target action | Psilocybin works by activating specific serotonin receptors, especially 5-HT2A and 5-HT1B. |
| Complex neuroplasticity | Mental health effects result from both acute and lasting changes in brain circuits. |
| Debated mechanisms | Scientists debate if one serotonin receptor explains all effects or if broader pathways matter too. |
| Focus on safe use | Reliable safety information prioritizes clinical research over informal claims about serotonin toxicity. |
| Personal growth potential | Therapeutic outcomes depend on both molecular mechanisms and subjective, contextual factors. |
What serotonin really does: Beyond ‘more equals better’
Serotonin is one of the brain’s most important chemical messengers, but it is wildly misunderstood in popular culture. The “low serotonin = depression” model, which drove decades of antidepressant marketing, has been thoroughly challenged by neuroscience. Serotonin does not simply make you feel happy when it goes up. It regulates mood, appetite, sleep, gut function, learning, and even how your brain processes incoming sensory information. The effect of serotonin on your brain depends less on how much of it is present and more on which receptors it is hitting and where in the brain those receptors are located.
Here is what makes serotonin’s role more nuanced than most guides admit:
- Serotonin has at least 14 distinct receptor subtypes, each triggering different cellular responses
- The same serotonin molecule can produce opposite effects depending on which receptor it binds
- Gut cells contain roughly 90% of the body’s serotonin, making it a whole-body signaling molecule
- Neuroplasticity, the brain’s ability to rewire itself, is tightly linked to serotonin signaling in key regions like the prefrontal cortex and hippocampus
This is where psilocybin gets genuinely interesting. Rather than increasing serotonin availability, psilocybin is converted in the body to psilocin, its active form. Psilocin then binds directly to serotonin receptors, particularly the 5-HT2A subtype. As noted in recent research, psilocybin is a serotonergic psychedelic whose active metabolite psilocin engages serotonin receptor signaling to drive both acute brain effects and longer-term neuroplasticity relevant to mental health outcomes.
That phrase, “longer-term neuroplasticity,” is the key. This is not just about how you feel during a session. It is about structural and functional changes in the brain that can persist for weeks or months after a single experience.
“Neuroplasticity is not just a buzzword. In the context of mental health, it describes the brain’s actual capacity to build new pathways, break old patterns, and update its default responses to stress, fear, and emotion.”
Understanding the psilocybin effects on mental health at this mechanistic level helps explain why its benefits are reported across such a wide range of conditions, from depression and PTSD to existential distress and addiction.
Pro Tip: When researching psilocybin, always check whether a source is talking about serotonin levels versus serotonin receptor activity. These are fundamentally different things with very different implications.
Now that you understand why the simple “serotonin boost” narrative falls short, let’s get specific about how psilocybin interacts with serotonin receptors.
Psilocybin’s action: Receptor-specific effects and neural pathways
Psilocybin does not hit one target and stop. Its active form, psilocin, interacts with multiple serotonin receptor subtypes, each contributing different pieces to the overall effect. But two receptors have attracted the most scientific attention: 5-HT2A and 5-HT1B.
The 5-HT2A receptor: Central to the classic psychedelic experience
The 5-HT2A receptor is psilocybin’s primary target, and it is highly concentrated in the prefrontal cortex, the brain region responsible for higher-level thinking, emotional regulation, and sense of self. When psilocin binds here, it disrupts the brain’s default mode network (DMN), the mental “autopilot” responsible for self-referential thinking, rumination, and rigid thought patterns.

Research confirms that activation of 5-HT2A receptors in specific circuits is the best-supported mechanism for psilocybin’s therapeutic effects, and that genetic disruption of these receptors in mice can completely abolish psilocybin’s long-term stress-behavior and structural plasticity effects.
That last point is critical. Remove the 5-HT2A receptor, and the therapeutic effect disappears. This is as close to a “smoking gun” as neuroscience gets.
The 5-HT1B receptor: A quieter but meaningful player
Emerging evidence points to 5-HT1B receptors as important modulators of psilocybin’s effects, particularly in cortico-claustrum circuitry. This network connects the cortex to a small but powerful brain region called the claustrum, thought to be involved in consciousness and sensory integration. Studies show that endogenous serotonin can modulate psilocybin-like network disruption through 5-HT1B receptors in this specific pathway, meaning your brain’s own serotonin interacts with psilocybin’s effects at this receptor.
Psilocin also demonstrates what researchers call polypharmacology, meaning it acts on multiple receptor subtypes simultaneously. As studies in animals have shown, 5-HT1B is functionally implicated in both acute and persisting behavioral effects of psilocybin, reinforcing that the full picture involves more than a single receptor.
Here is a simplified comparison of the two primary receptors in question:
| Receptor | Location | Primary role | Evidence strength |
|---|---|---|---|
| 5-HT2A | Prefrontal cortex, cortex | Disrupts DMN, drives neuroplasticity | Very strong (genetic knockout abolishes effects) |
| 5-HT1B | Cortico-claustrum circuits | Modulates network disruption, influences acute effects | Emerging but growing |
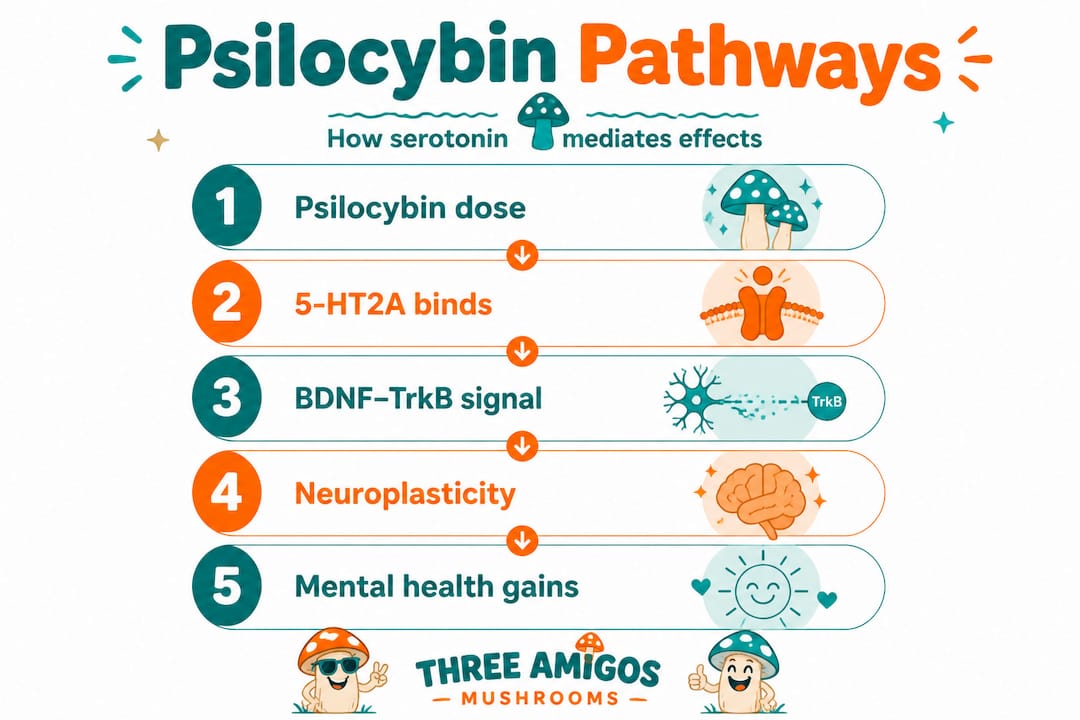
The numbered sequence of events at the receptor level looks roughly like this:
- Psilocybin is ingested and converted to psilocin in the liver
- Psilocin crosses the blood-brain barrier and binds to 5-HT2A receptors in the prefrontal cortex
- This disrupts the default mode network and triggers altered patterns of brain connectivity
- Downstream signaling pathways, including neurotrophic (brain growth) factors, are activated
- 5-HT1B receptors in cortico-claustrum circuits modulate how strongly the disruption registers
- Over days and weeks, structural plasticity changes consolidate, potentially rewiring stress response patterns
Understanding these mechanisms is central to appreciating psilocybin and neuroplasticity, which is the foundation for its mental health applications. For a broader view of the psychedelic neuroscience behind these effects, going deeper into the circuit-level research is worth your time.
Understanding receptor-level specificity gives us the framework, but science actively debates how these actions translate into longer-term mental health outcomes.
Debates and breakthroughs: Is 5-HT2A enough to explain everything?
Here is where the science gets genuinely contested, and where anyone interested in mental health applications should pay close attention.
Even though 5-HT2A activation is considered essential, there is real scientific disagreement about whether this receptor alone drives psilocybin’s lasting therapeutic effects. Current reviews highlight active debate over whether 5-HT2A signaling is required for neuroplastic effects, with conflicting data motivating the development of new mechanistic models. This is not a minor footnote. If the neuroplasticity effects do not fully require 5-HT2A, that changes how we think about predicting who responds to treatment and why.
The BDNF–TrkB pathway: A convergence point
One reason 5-HT2A may not be the whole story involves a signaling pathway called BDNF-TrkB. BDNF (brain-derived neurotrophic factor) is essentially fertilizer for neurons. TrkB is its receptor. When BDNF binds TrkB, it triggers neural growth and strengthening of synaptic connections, which is a key mechanism in mood regulation and resilience.
Research suggests that shared downstream pathways like BDNF-TrkB may converge on therapeutic outcomes even when serotonergic targets differ, supporting a systems-level view rather than a single-receptor model. Interestingly, ketamine, a completely different compound that works on NMDA glutamate receptors rather than serotonin receptors, activates the same BDNF-TrkB pathway. This convergence suggests that different substances may arrive at similar therapeutic destinations through different routes.
Here is a high-level look at how these pathways compare:
| Compound | Primary receptor | Downstream plasticity pathway | Subjective experience required? |
|---|---|---|---|
| Psilocybin | 5-HT2A, 5-HT1B | BDNF-TrkB, mTOR signaling | Debated but likely yes |
| Ketamine | NMDA (glutamate) | BDNF-TrkB | Appears less critical |
| SSRIs | Serotonin transporter | BDNF upregulation (slow) | Not applicable |
Key takeaways from the ongoing debates:
- A single receptor model is almost certainly too simple
- Shared plasticity pathways might explain why different compounds can produce similar antidepressant outcomes
- The subjective experience during a psilocybin session may itself contribute to neuroplastic changes, not just the receptor binding
- Dose, setting, preparation, and individual genetics all interact with receptor-level effects
Pro Tip: If you encounter a source claiming one mechanism is the definitive explanation for psilocybin’s therapeutic effects, treat that as a red flag. The best researchers in this field are the ones acknowledging what they still do not know.
This is precisely why the research on depression remission from psilocybin trials is so compelling, but also why it needs to be interpreted carefully. The science around psilocybin’s effects is advancing fast, but it is not yet a closed case.
Implications for mental health, personal growth, and safety
Connecting all of this receptor science to your actual life is where things get practical. Here is what the molecular evidence means for people in Canada who are exploring psilocybin for real purposes.
Mental health applications are the most studied area. Psilocybin’s effects on the default mode network, combined with downstream neuroplasticity through BDNF-TrkB, create conditions where entrenched patterns of thinking, anxiety responses, and depressive rumination can be temporarily loosened and reorganized. This is not magic, and it is not guaranteed. Context, intention, and support structures significantly shape outcomes.
Personal growth beyond clinical settings is a legitimate area of interest. Neuroplasticity does not only matter for treating diagnosed conditions. Improved cognitive flexibility, emotional regulation, and openness to new perspectives are documented effects that many people seek outside of clinical trials. The molecular basis for these outcomes is the same receptor signaling we have been discussing.
Important safety points to keep in mind:
- Psilocybin does not combine safely with serotonin syndrome risk compounds without careful evaluation. While pharmacovigilance research notes that serotonin toxicity concerns exist in the literature, reliable risk assessment requires consulting clinical or medical literature, not informal blogs
- People on SSRIs or lithium should consult a knowledgeable healthcare provider before using psilocybin
- Set and setting, your mindset and physical environment, are not soft variables. They interact with the neurological mechanisms and shape outcomes
- Dosing matters enormously. Microdosing and macrodosing produce very different receptor activation profiles
“The receptor story matters, but it does not happen in a vacuum. Your emotional state, your environment, your intention, and your support system are all part of the system that psilocybin interacts with.”
The concept of a psilocybin entourage effect is relevant here. Just as with cannabis, the interplay of multiple active compounds and biological systems may produce effects that no single molecule or receptor can fully account for.
Why most guides miss the real point about serotonin and psilocybin
Here is what we genuinely believe after following this science closely: the serotonin conversation in the public sphere is stuck at the wrong level of analysis. People argue about whether serotonin goes up or down, whether one receptor matters more than another, or whether psilocybin is “just like an antidepressant but faster.” All of these framings miss the bigger picture.
The more useful question is not which receptor psilocybin hits, but how receptor activation reorganizes networks and whether the person in the experience can use that window of plasticity productively. Evidence from clinical research confirms that therapeutic effects likely depend on both subjective experience and downstream plasticity processes in interacting networks. This is a systems-level insight, not a simple chemical one.
For Canadians specifically, this matters because regulatory frameworks and public safety conversations tend to lag behind the actual science. Staying grounded in mechanistic, peer-reviewed evidence rather than social media summaries or sensationalist headlines is genuinely protective. It helps you evaluate products, dosing approaches, and claims from vendors or wellness influencers more critically.
We also think it is worth naming something that rarely gets said in these conversations: not everyone benefits from psilocybin, and not every difficult experience produces growth. The serotonergic mechanism is real, the plasticity data is compelling, and the clinical results are genuinely exciting. But the individual response is shaped by factors that no receptor chart can fully predict. Respecting that complexity is not pessimism. It is good science. For a broader foundation, the psilocybin science explained resource we have built digs into many of these layers in accessible detail.
Learn and explore psilocybin’s benefits safely in Canada
Bridging the gap between receptor-level science and your own experience starts with access to reliable information and quality products you can actually trust.
At Three Amigos, we have built our platform around both: a deep library of evidence-based psilocybin science and a curated selection of products for Canadians who want to explore thoughtfully. Whether you are starting with microdosing capsules designed for consistent, low-dose receptor engagement or working toward a more intentional full-dose session, we offer options built on quality assurance and harm-reduction principles. Our microdosing benefits guide walks through the science in practical, digestible terms for anyone ready to take an informed next step.
Frequently asked questions
Which serotonin receptors are most important for psilocybin’s effects?
Psilocybin mainly acts on the 5-HT2A receptor and the 5-HT1B receptor, each shaping distinct brain and behavioral outcomes, with 5-HT2A being the most strongly supported for therapeutic effects.
Does psilocybin simply increase serotonin?
No. Psilocin directly stimulates serotonin receptors, especially 5-HT2A, without raising overall serotonin levels in the brain.
Are all psilocybin’s mental health effects explained by 5-HT2A activation?
Not entirely. Newer research shows that shared plasticity pathways like BDNF-TrkB and other receptor subtypes also contribute to its therapeutic outcomes.
Is there a risk of serotonin syndrome with psilocybin use?
Clinical research does not confirm clear serotonin syndrome risk from psilocybin alone, but pharmacovigilance sources should be consulted rather than informal online claims, especially for people on serotonergic medications.
How does psilocybin promote personal growth?
Psilocybin’s action on neuroplasticity and the subjective experience it generates work together. Clinical evidence shows that outcomes depend on both molecular changes and the quality of the individual’s experience during the session.
Recommended
- Psilocybin science explained: unlock mental health benefits
- Psilocybin Research Explained: Mental Health Impacts
- Psilocybin’s entourage effect and mental health benefits
- Psilocybin effects: mental health and personal growth
Thomas Wrona is a writer, designer, and wellness coach who believes that nature’s wisdom provides an antidote to the stress of modern life. As a former pro athlete, he’s all about staying in motion! When he’s not writing you’ll probably find Thomas outside.





